What Is Stress Incontinence?
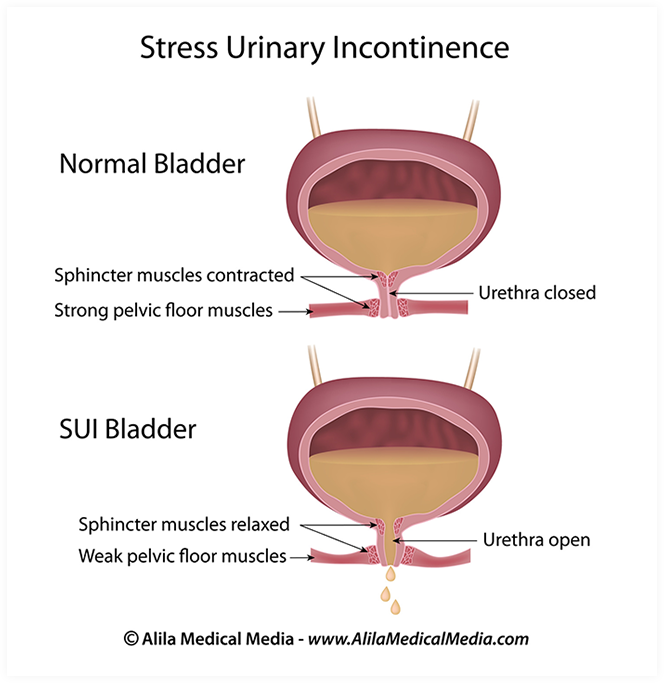
Stress incontinence occurs when urine leaks during activities like laughing, coughing, sneezing, or exercising. It happens when pressure on the bladder overcomes the mechanisms that keep the bladder neck closed, including:
- Internal Sphincter: A muscle at the bladder neck that normally prevents leakage.
- Collagen Support: Tissue around the urethra aiding closure.
- Pelvic Floor Muscles: External muscles supporting the urethra, relaxing only during urination.
Dr. Kumar offers expert evaluations to diagnose stress incontinence and create a tailored treatment plan.
Causes of Stress Incontinence
Stress incontinence results from weakened bladder support, allowing urine to leak under pressure. Common causes include:
- Pregnancy and Childbirth: Stretching and weakening pelvic floor muscles.
- Menopause: Reduced collagen and blood supply to the urethra.
- Weight Gain: Increased pressure on the bladder and pelvic floor.
- Vigorous Exercise: Straining from high-impact activities.
- Genetic Factors: Inherently weaker collagen in some women.
Dr. Kumar uses advanced diagnostics to identify the specific cause of your symptoms.
Treatment Options
Dr. Kumar tailors treatments based on a thorough evaluation, addressing related conditions like overactive bladder or recurrent UTIs. Options include:
- Pelvic Floor Physical Therapy: Guided exercises with a specialist, more effective than solo Kegels.
- Intravaginal Devices: Support the bladder neck to reduce leaks.
- Collagen Restoration: In-office procedures to rebuild collagen in the bladder neck and vaginal walls.
- Urethral Injections: Fillers to add volume and create a tighter urethral seal.
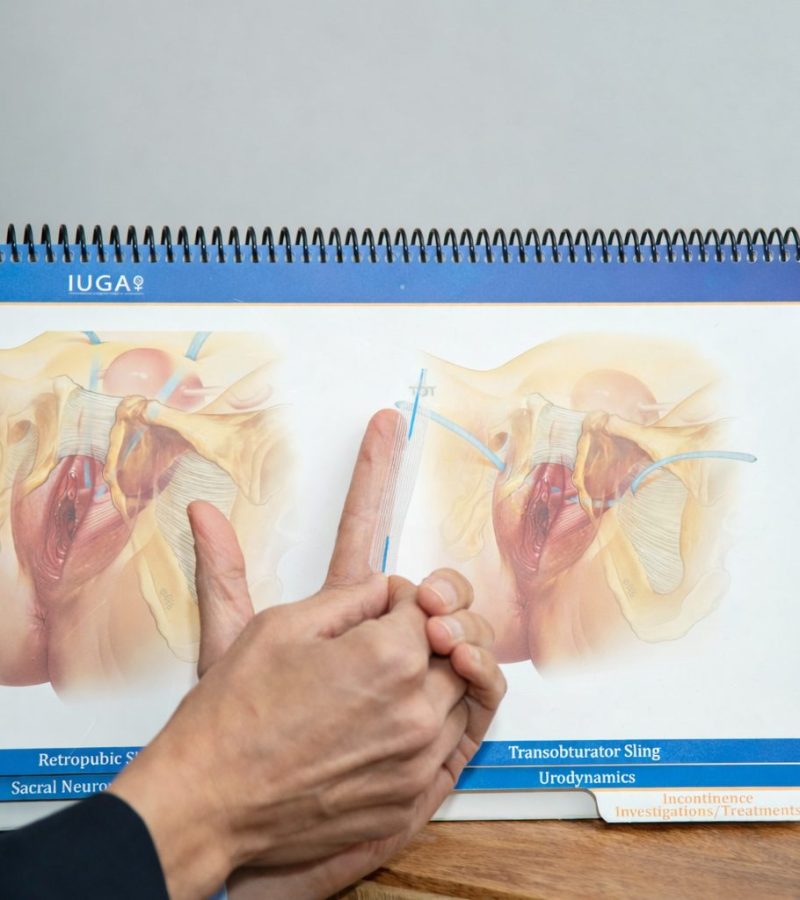
- Sling Surgery: A highly effective (80-90%) surgical option for severe cases.
Treatments may also address menopausal symptoms or lifestyle factors for comprehensive care.
Common Questions & Answers
Stress incontinence is caused by weakened pelvic floor muscles, reduced collagen (often due to menopause), pregnancy, childbirth, weight gain, vigorous exercise, or genetic factors affecting collagen strength.
Yes, it’s extremely common, especially after childbirth or during menopause, with leaks during activities like laughing, coughing, or exercising.
Guided pelvic floor therapy with a specialist can significantly improve symptoms. Solo Kegels are less effective, but Dr. Kumar may recommend devices for better results.
Urethral injections use fillers to add volume inside the urethra, creating a tighter seal to prevent leakage. They’re minimally invasive, done in-office, and ideal for mild to moderate cases.
Sling surgery, effective in 80-90% of cases, is considered if conservative treatments like therapy, devices, or injections don’t provide enough relief. Dr. Kumar personalizes recommendations.