What Is Overactive Bladder?
Overactive bladder (OAB) is a common condition affecting 40% of women and 1 in 6 adults in the U.S., causing frequent, sudden urges to urinate—often every 2–3 hours. When leakage occurs before reaching the bathroom, it’s called urge incontinence. OAB disrupts daily life, impacting activities and confidence.
- Frequent Urges: Needing to urinate more than 8 times daily or multiple times at night.
- Urgency: Sudden, strong urges that are hard to delay.
- Urge Incontinence: Leaking urine before reaching the toilet.
Dr. Kumar offers expert evaluations to diagnose OAB and create a tailored treatment plan.

Causes of Overactive Bladder
OAB can result from various factors that affect bladder function. Common causes include:
- Nerve Signal Issues: Miscommunication between the brain and bladder.
- Hormonal Changes: Menopause-related shifts weakening bladder control.
- Pelvic Floor Muscles: Weak or overactive muscles impacting urine storage.
- Medications: Side effects from certain drugs causing bladder irritation.
- Neurologic Conditions: Conditions like multiple sclerosis, stroke, or spinal cord injuries (diagnosed as neurogenic OAB).
Dr. Kumar uses advanced diagnostics to identify the specific cause of your OAB symptoms.
Treatment Options
We offer personalized, evidence-based treatments for OAB, tailored to your symptoms and lifestyle:
- Medications: Prescription drugs to relax the bladder and reduce urgency.
- Bladder Botox: In-office injections to calm overactive bladder muscles.
- PTNS (Percutaneous Tibial Nerve Stimulation): Gentle nerve stimulation near the ankle to improve bladder control.
- Sacral Nerve Stimulation (SNS): A minimally invasive device to restore bladder-brain communication (see our SNS page).
If conservative treatments like pelvic floor therapy fail, Dr. Kumar provides advanced, minimally invasive options with proven results.
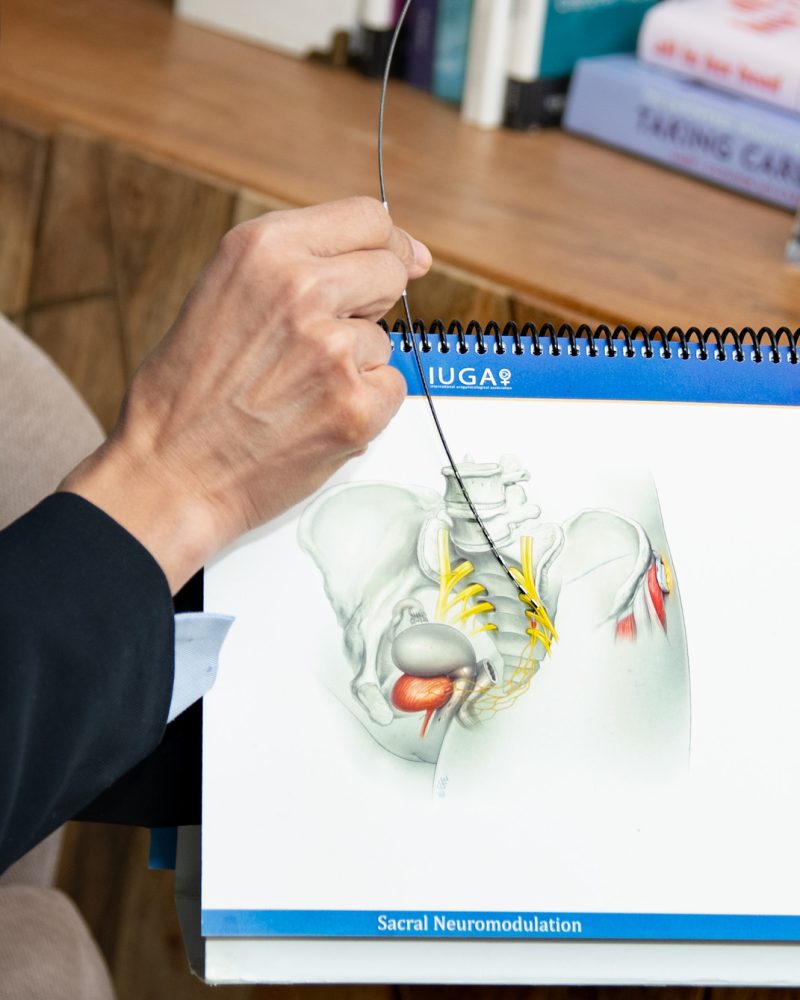
Common Questions & Answers
OAB can often be managed effectively with therapies, lifestyle changes, or neuromodulation. Many women achieve long-term relief with the right treatment plan.
Urge incontinence, linked to OAB, involves sudden, uncontrollable urges to urinate. Stress incontinence occurs during physical activities like coughing or exercising due to weak pelvic muscles.
Most OAB cases are treated non-surgically with medications, Botox, or nerve stimulation. Surgery is rarely needed, and Dr. Kumar prioritizes minimally invasive options.
Yes, hormonal changes during menopause or pelvic strain from childbirth can contribute to OAB. Dr. Kumar offers targeted treatments to address these triggers.
Dr. Kumar may use symptom evaluations, bladder diaries, or urodynamics testing to diagnose OAB and identify whether nerve issues or muscle dysfunction are the cause.